Archival Notice
This is an archive page that is no longer being updated. It may contain outdated information and links may no longer function as originally intended.
Home | Glossary | Resources | Help | Contact Us | Course Map
Surfaces
Household bleach is 5.25% sodium hypochlorite (52,500ppm), so a 1% bleach solution is 525ppm and sufficient for inactivating most viruses. Per the Centers for Disease Control and Prevention (CDC), chlorine solutions gradually lose strength, so diluted solutions should be replaced daily.01 Some laboratories have changed from the traditional 10% mix in a bottle to a type of container that mixes neat bleach and water at the time it is expressed from the bottle. Biocidal activity is affected by the presence of organic material, which consumes available chlorine. Some laboratories may employ a detergent based germicidal disinfectant, e.g. Coverage Plus®, or a decontaminant such as DNA Away™ per manufacturer's directions. Cleaning with bleach or detergents may be followed by water and/or EtOH to eliminate the possibility of introducing bleach or detergent into the sample or build up. EtOH alone, even 70% as employed in microbiology settings to prevent transfer of pathogens, is not sufficient to rid a surface of exogenous DNA.
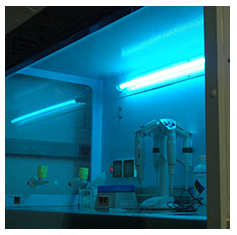
Another means of decontaminating hoods, reagents, pipettes, tubes, etc., is exposure to UV light. Most biological safety cabinets are equipped with a UV light source. It is generally accepted that UV exposure at 254nm for a minimum of 5 minutes is sufficient for disinfection to include the deactivation of nucleases and destruction of extraneous DNA on surfaces. Laboratory SOPs often include UV exposure steps as long as 30 minutes before and after use of hoods for PCR work. Wiping with bleach and/or detergents is still warranted as the penetrating power of UV light is minimal.
Reagents, Consumables, and Tools
Applicable consumables and tools such as scissors, microcentrifuge tubes, spin baskets, racks, glassware, containers, and other items may be autoclaved. Many laboratories, as a part of their quality control program, autoclave some reagents prior to use, and may prepare some reagents from autoclaved solutions. It is a good practice to apply autoclave tape to items being sterilized to test the autoclave's efficacy and differentiate between items that have and have not been autoclaved. Laboratories should pay careful attention to the plastics used in the laboratory if they are to be autoclaved, as some can break down, becoming more porous and prone to harboring contaminants. When using tubes or supplies that have been autoclaved in a container, it is good laboratory practice to pour them onto a clean surface rather than reaching into the container to retrieve them.
- U.S. Department of Health and Human Services Centers for Disease Control and Prevention and National Institutes of Health. 1999. Biosafety in microbiological and biomedical laboratories. 4th ed. Washington, D.C.: U.S. Government Printing Office (accessed August 31, 2006).
Additional Online Courses
- What Every First Responding Officer Should Know About DNA Evidence
- Collecting DNA Evidence at Property Crime Scenes
- DNA – A Prosecutor’s Practice Notebook
- Crime Scene and DNA Basics
- Laboratory Safety Programs
- DNA Amplification
- Population Genetics and Statistics
- Non-STR DNA Markers: SNPs, Y-STRs, LCN and mtDNA
- Firearms Examiner Training
- Forensic DNA Education for Law Enforcement Decisionmakers
- What Every Investigator and Evidence Technician Should Know About DNA Evidence
- Principles of Forensic DNA for Officers of the Court
- Law 101: Legal Guide for the Forensic Expert
- Laboratory Orientation and Testing of Body Fluids and Tissues
- DNA Extraction and Quantitation
- STR Data Analysis and Interpretation
- Communication Skills, Report Writing, and Courtroom Testimony
- Español for Law Enforcement
- Amplified DNA Product Separation for Forensic Analysts